Pericardial Window
Medically reviewed by Drugs.com. Last updated on Jun 5, 2024.
AMBULATORY CARE:
What you need to know about pericardial window (PW):
PW is surgery to drain extra fluid from the protective sac around your heart (pericardium). The extra fluid puts pressure on your heart. This makes it hard for your heart to work properly.
How to prepare for PW:
- Your surgeon will tell you how to prepare. Your surgeon may tell you not to eat or drink anything after midnight on the day of your surgery. Arrange to have someone drive you home when you are discharged.
- Tell your surgeon about all medicines you currently take. Your surgeon will tell you if you need to stop any medicine for the surgery, and when to stop. Your surgeon will tell you which medicines to take or not take on the day of surgery.
- Tell your surgeon about any allergies you have, including medicines or anesthesia. You may be given an antibiotic to help prevent a bacterial infection.
- You may need blood and urine tests before your surgery. These tests show how well your kidneys are functioning and your blood is clotting. You may need an EKG, a chest x-ray, or an echocardiogram. A CT, MRI, or heart catheterization may also be needed.
What will happen during PW:
- In most cases you will be given general anesthesia. This type of anesthesia will keep you asleep and free from pain during surgery. You may be given local anesthesia to numb the surgery area. With local anesthesia, you may feel pressure or pushing, but you should not feel any pain.
- There are several ways to do this surgery. Your surgeon may make an incision below your breastbone. Instead, one or more small incisions may be made between your ribs. Several smaller incisions will be made on the side of your chest if your surgeon uses a scope. The scope and other small instruments will be inserted through these incisions.
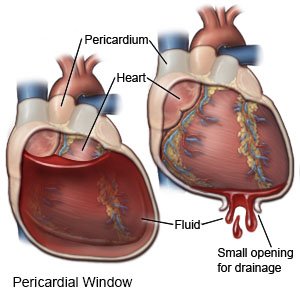
- Your surgeon will remove a small piece of the sac around your heart. This will allow the extra fluid to drain. A shunt, or hollow tube, may be placed. This keeps the area open and prevents another build up of extra fluid. A sample of the fluid or the sac may be collected for more testing. A chest tube may be placed to help drain the extra fluid. Your incisions will be closed with staples, stitches, medical tape, or medical glue.
 |
What to expect after PW:
You may have mild pain or discomfort for a few days. You may have a chest tube draining extra fluid from your heart or chest. You may need to stay in the hospital for a few days. You may need an echocardiogram before you are discharged from the hospital. This test shows new build up of fluid after your surgery.
Risks of PW:
You may bleed more than expected or get an infection. Your heart may be damaged during the surgery. Extra fluid may build up around your heart again. You may need to have another heart surgery. You may have an abnormal heart rhythm or heart attack. The ability of your heart to function properly may be decreased. This can lead to heart failure.
Call your local emergency number (911 in the US), or have someone call if:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
- You have any of the following signs of a stroke:
- Numbness or drooping on one side of your face
- Weakness in an arm or leg
- Confusion or difficulty speaking
- Dizziness, a severe headache, or vision loss
- You feel lightheaded, short of breath, or have chest pain.
- You cough up blood.
- You have trouble breathing.
Seek care immediately if:
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- Blood soaks through your bandage.
- Your incision comes apart.
Call your cardiologist or doctor if:
- You have a fever or chills.
- Your incision site is red, swollen, or draining pus.
- You have nausea or are vomiting.
- Your skin is itchy, swollen, or you have a rash.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Care for your surgery area as directed:
Carefully wash around the area with soap and water. Do not scrub. Let the soap and water run over the area. If you do not have a bandage, gently pat the area dry with a clean towel. If you have a bandage, dry the area and put on a new, clean bandage. Change your bandage if it gets wet or dirty. Check the area for signs of infection, such as redness, swelling, or pus.
Activity:
Your surgeon will give you specific activity instructions. You may need to limit activity for a certain amount of time. You may not be able to lift anything over a certain weight. Your surgeon will tell you when you can drive, go back to work, or do other activities.
Follow up with your doctor or cardiologist as directed:
You may need to return to have your stitches or staples removed. You may also need more tests, such as an echocardiogram. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2024 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
