Panretinal Photocoagulation
Medically reviewed by Drugs.com. Last updated on Jul 7, 2024.
AMBULATORY CARE:
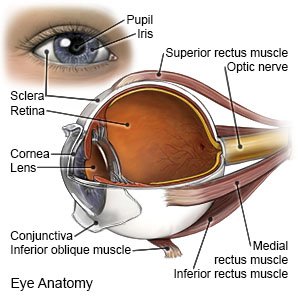
Panretinal photocoagulation (PRP)
is a procedure used to treat leaking blood vessels in the retina. Certain conditions weaken the blood vessels, causing them to leak. Proliferative diabetic retinopathy is the most common condition PRP is used to treat. This condition causes the retina to create new, weak blood vessels that also leak. PRP makes hundreds of tiny burns that seal leaking vessels on the peripheral (outer) part of the retina. New vessels are also prevented from growing. PRP will not give you back lost vision, but it can keep vision loss from getting worse.
 |
How to prepare for PRP:
- Your healthcare provider will tell you how to prepare. Arrange to have someone drive you home after the procedure. You may need to have more than one treatment. Make sure you arrange to have someone drive you home after each treatment session.
- You may be asked to bring dark sunglasses to your PRP appointment. Your pupils will be dilated (widened) to help your provider see your retina more easily. Your pupils will absorb more harmful sunlight than usual while they are dilated. You will need to wear the dark sunglasses during your ride home. You also need them when you are outside until your pupils go back to their normal size.
- Tell your provider about all medicines you currently take. He or she will tell you if you need to stop any medicine for the procedure, and when to stop. He or she will tell you which medicines to take or not take on the day of the procedure.
What will happen during PRP:
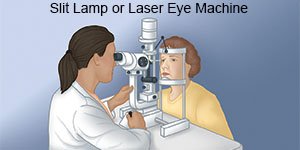
- You may be given local anesthesia as eyedrops or shots to help prevent discomfort. You may still feel a mild ache during the procedure, but you should not feel pain. A contact lens will be placed on your cornea. The lens will keep your eye still and help the laser focus.
- The machine used for the procedure is similar to the machine used during a regular eye exam. You will sit with your chin on the chinrest and your forehead against the headrest. You may be asked to look at a target with the eye that is not being treated. This helps you keep your treated eye where your provider wants it during treatment.
- The laser will be directed at many blood vessels in the peripheral (outer) part of the retina. You may see flashes of bright light during the procedure. Tell your provider if you feel severe pain while the laser is being used. He or she may need to make changes to your procedure.
- Anti-vascular endothelial growth factor (anti-VEGF) treatment may be given to reduce swelling and improve vision. Medicine is injected into the vitreous of the eye. The vitreous is the gel-like material that fills the inside of the eye.
 |
What to expect after PRP:
- You should be able to return to most activities right away.
- You may feel a mild ache in your eye or see flashes of light for a day or two.
- Your vision may be blurry for up to a week.
- You may have a headache for a few hours.
Risks of PRP:
You may have heavy bleeding in your eye, or your retina may become detached (pulled away). You may have temporary or permanent blurred vision, vision loss, double vision, or peripheral vision problems. You may have trouble driving at night. You may not see color or contrast as well as before PRP. Your eyelid may droop. New blood vessels may grow, and you may need PRP to control the growth. PRP can also cause edema that puts pressure on blood vessels. The pressure can cause more leaking that leads to vision loss. You may still lose your vision even with successful PRP.
Call your local emergency number (911 in the US) if:
- You suddenly cannot see.
Seek care immediately if:
- Your vision seems covered by a dark curtain.
- You have severe eye pain.
- You have more trouble seeing.
Call your doctor or ophthalmologist if:
- You have new or worsening vision problems.
- You continue to have a headache after 2 days.
- You have questions or concerns about your condition or care.
Acetaminophen
decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
Do not drive, as directed:
Your vision may be affected for several days. You may not be able to see out of the sides of your eyes (peripheral vision). This can make safe driving difficult. Ask someone to drive you until your healthcare provider says it is okay to drive.
Protect your vision:
- Get an eye exam as often as directed. Eye exams are usually done every 2 to 3 months to monitor proliferative diabetic retinopathy. If you have diabetic macular edema, you may need exams every 4 to 6 weeks. Early diagnosis and treatment of eye problems may prevent permanent vision damage.
- Manage health conditions that can cause vision problems. Common examples include diabetes, high blood pressure, and high cholesterol. Follow up with healthcare providers who manage these conditions.
- Wear sunglasses with ultraviolet (UV) light protection. UV light from the sun can damage your eyes. It can increase your risk for vision loss.
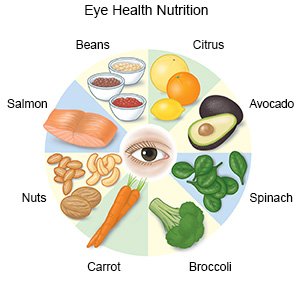
- Eat foods that contain eye-healthy nutrients. Healthy nutrients include vitamin A, vitamin C, vitamin E, omega-3 fatty acids, lutein, and zeaxanthin. They can be found in foods such as spinach, peanuts, salmon, collard greens, avocados, squash, eggs, and blueberries. Ask your healthcare provider for a full list of foods that contain eye-healthy nutrients. You may also need to take a vitamin or supplement to help you get enough of these nutrients.
- Exercise as directed. Ask your healthcare provider about the best exercise plan for you. He or she will tell you how to control your blood sugar level when you exercise. You may need to check the level more often during exercise. Bring a snack with you when you exercise in case your blood sugar level gets too low.

- Do not smoke. Nicotine can damage blood vessels in your eyes. Do not use e-cigarettes or smokeless tobacco in place of cigarettes or to help you quit. They still contain nicotine. Ask your healthcare provider for information if you currently smoke and need help to quit.
Follow up with your doctor or ophthalmologist as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2024 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
