Understanding Opioid (Narcotic) Pain Medications
Narcotics, also called opioids, are a necessary and important part of medical care. Many painkillers, medically known as narcotic analgesics, contain some type of opioid medication to ease the discomfort from conditions such as a sprained ankle, after wisdom tooth extraction, or after major surgery. For many types of acute pain, a non-opioid, like acetaminophen or an NSAID may be as effective as an opioid.
Opioids are also used as a cough suppressant, to treat diarrhea and to help combat narcotic addiction itself. However, the use of prescription opioids for pain is now a highly controversial topic in the U.S. due to a growing epidemic of prescription narcotic addiction, overdose, and death.
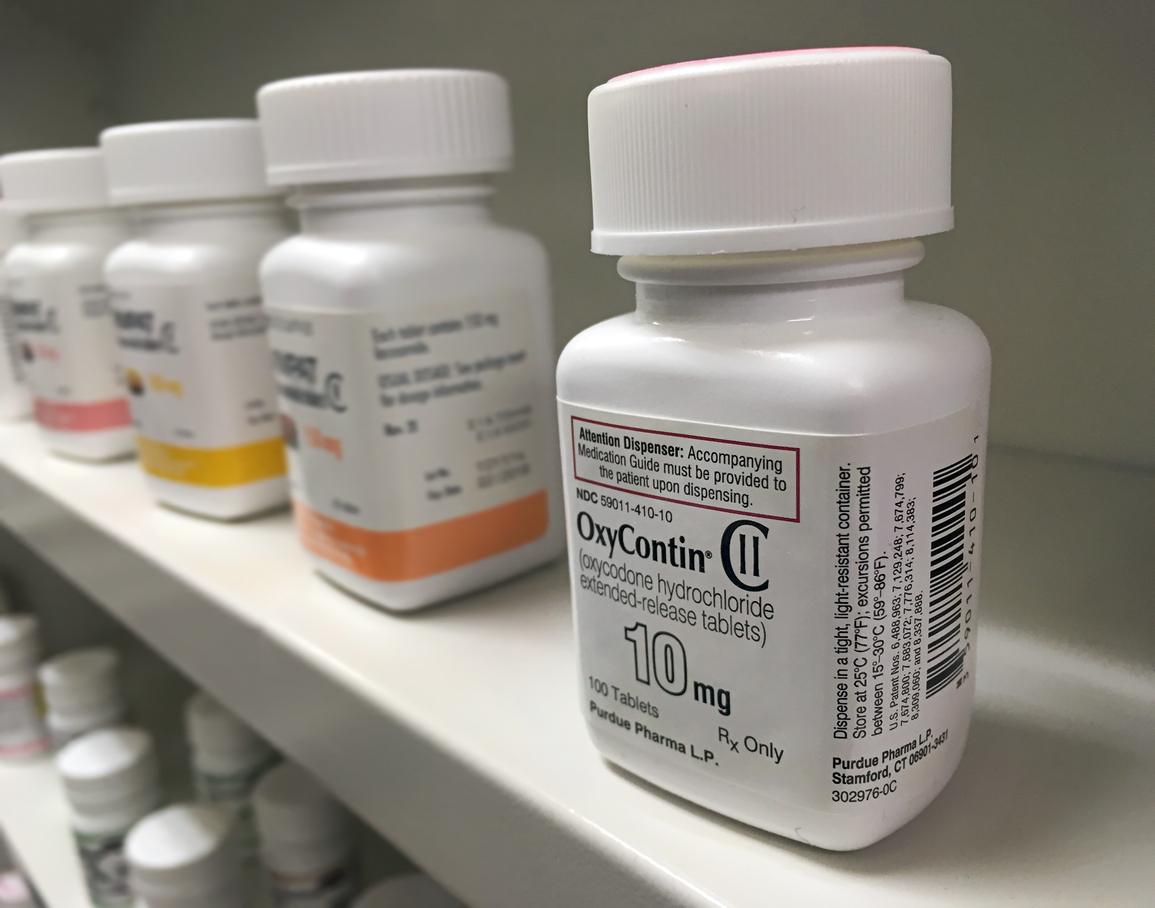
We’ve all been prescribed opioid prescription painkillers from time-to-time, and the choices are many. You’ve heard of their names: oxycodone (Oxycontin) , hydrocodone, tramadol (Conzip, Qdolo, Ultram), and many others.
But what are opioids and what if we need to take them for a legitimately painful condition? Here’s some detailed history of opioids to help you better understand painkillers, their prescribing information, and the current concerns about addiction.
- A Brief History of Narcotics
- What Is a Narcotic Medication?
- How Do Narcotics Work?
- What Kind of Pain Does a Narcotic Treat?
- Is My Drug a Narcotic?
- List of Prescription Narcotic Drugs (Single Agents)
- List of Prescription Narcotic Drugs (Combination Agents)
- Common Uses for Prescription Narcotics
- Common Side Effects of Narcotics
- The FDA Response to Narcotic Addiction
- Rescheduling of Narcotics to Ease Misuse and Diversion
- Can I Become Addicted to a Prescription Narcotic Painkiller?
- What is Naloxone (Narcan)?
- Popular Culture and Drug Use
- Drug Testing for Narcotics
History of Opioids
Ancient Times
Narcotics, also known as opioids, date back to 3400 B.C. Narcotics from ancient times all had a common source: the red opium poppy.
The earliest records of the opium poppy being cultivated was in Mesopotamia by the Sumerians. The Sumerians referred to opium as the “joy plant” and passed it on to the Egyptians. Around 400 B.C. the first medical references to opium came from Hippocrates, also known as the Father of Medicine.
The Middle Ages
- Oddly, opium disappeared from the European records up until around 1500, so documentation is sparse. However, in the early 1500’s Paracelsus, the first toxicologist, created an opium pill also using citrus juice and gold.
- Paracelsus also made a specific tincture (alcoholic extract) of opium called “laudanum”, from the latin meaning “to praise”.
- Laudanum contains roughly 10% powdered opium by weight, equivalent to 1% morphine.
The 19th and 20th Century
In the 1800’s opium was recognized as a standard painkiller when morphine was isolated from the poppy. German chemist Friedrich Wilhelm Adam Serturner dubbed the isolate “morphine” after the Greek god of dreams, Morpheus.
Opiuim, morphine and heroin addiction had become a major problem by the early 1900’s and during the civil war. Congress starting imposing regulations to restrict opium.
- The Opium Exclusion Act of 1909: Barred importation of opium for purposes of smoking
- The Harrison Narcotics Tax Act of 1914: Required physician and pharmacist registration for distribution of opiates
- The Heroin Act of 1924: Heroin importation, manufacture and possession was outlawed in the U.S.
Bayer stopped the production of heroin but in 1916 oxycodone was developed in hopes it would be less addictive.
In 1938, the Food, Drug and Cosmetic Act was passed that required all medications to be proven as safe by the FDA; however, older opioid-derived drugs such as morphine, codeine, and oxycodone were “grandfathered” meaning they were automatically allowed without further review.
Fast-forward to the 1950’s, 1960’s, and 1970’s and that’s where the more familiar opioids like Percodan (oxycodone and aspirin) start to gain hold in the U.S. market. Since this time, the illegal abuse of semi-synthetic and synthetic narcotics has been a growing problem in the U.S.
With the passage of the Controlled Substances Act (CSA) in 1970, greater regulation and scheduling of drugs based on abuse potential occurred.
- Within the CSA there are five schedules (I-V) that are used to classify drugs based upon their potential for abuse, valid medical applications, and public safety.
- The schedules range from I to V, with schedule I being the highest for potential abuse and with no current medical use.
- Heroin and marijuana fall into schedule 1; oxycodone, hydrocodone and morphine are in schedule 2. Marijuana still remains schedule 1 at the federal level, although several states in the US have now legalized recreational and medicinal use of cannabis.
The Drug Enforcement Agency was created in 1973, and President Nixon declared ‘The War on Drugs’ noting the high incidence of heroin addiction in the U.S.
The 21st Century
In the first decade of 2000, a new emphasis on medical control of pain was emphasized by healthcare policy makers and pharmaceutical industry, leading to an explosion in opioid prescribing. Brands such as:
were overprescribed, leading to millions of addicted patients and emergency department visits due to painkillers and overdose. The pharmaceutical industry began research into development of abuse-deterrent formulations of opioid medications, many of which are now available on the U.S. market.2,3 However, none of these forms prevent abuse by simply taking the medication by mouth.
The true effect of abuse-deterrent opioids on the reduction of narcotic overdose and death is not yet known. In fact, it will probably take a multi-pronged approach to defeat the epidemic of narcotic abuse in this country, including availability of naloxone (Narcan Nasal, Kloxxado, Zimhi) for overdose, patient and provider education, effective legislation, and easily available treatment options for addiction.
Learn More: CDC Clinical Practice Guideline for Prescribing Opioids for Pain - United States, 2022
What Is a Narcotic Medication?
It’s important to define "narcotic" in a medical sense. The word “narcotic” often denotes a negative connotation associated with illegal drugs and addiction. While this can be true, “narcotic” is also a standard term used in medicine.
- A narcotic drug, also called a narcotic analgesic or opioid, is a medication prescribed by a doctor to relieve moderate to severe pain, either acute (short-term) or chronic (longer-term or continuous) pain.
- Narcotic analgesics differ in their ingredients, strengths, dosage forms, and cost. Many are available as oral tablets, capsules, or liquids, while some come as an injection, and others are provided as a patch to provide extended-release control for severe pain.
How Do Narcotics Work?
Overall, narcotic painkillers work by reducing nerve excitability that leads to the sensation of pain.
Narcotics bind to special receptors in the brain (central nervous system) and in other areas of the body (peripheral nervous system, like the gastrointestinal tract) called opioid receptors. There are four types of opioid receptors: mu, delta, kappa, opioid receptor like-1 (ORL1).
These receptors either aid with the opening of potassium channels (causing hyperpolarization) or block calcium channel openings and the release of excitatory neurotransmitters like substance P that are involved with pain.
Sometimes a painkiller drug may be referred to as a “narcotic-like” medicine, but any true narcotic medication will have action at one of these opioid receptors.
Tramadol is often referred to as a “narcotic-like” medication suggesting it may be safer, but this is not really true. It has centrally-acting analgesic action at the opioid mu receptors, blocking pain pathways like regular opioids. Tramadol is also thought to act via weak reuptake inhibition of norepinephrine and serotonin, and this may add to its pain effects. In addition, tramadol pain relief is partially blocked by the opiate antagonist naloxone in animal studies.4,5
Tramadol is a classified as a controlled substance in schedule IV. Schedule IV drugs have the potential for abuse and dependence, but this potential is lower than other narcotic analgesics in schedule II or III (for example, morphine or buprenorphine).
What Kind of Pain Does a Narcotic Treat?
There are literally hundreds of pain conditions where narcotic analgesics could be used to lessen discomfort.
- Guidelines suggest to use non-drug therapy and non-opioid medication when possible to control acute, non-cancer pain. The latest 2022 CDC guidelines leave the determination of opioid use to shared decision making between clinician and patients.
- Opioids for acute pain should only be used short-term to help prevent dependence and addiction. Once the severe acute pain subsides other non-narcotic medications such as acetaminophen or ibuprofen may be suitable for longer-term use.
- The doctor and patient should develop a plan for pain control early in the treatment course, and agree on a timeline to stop the opioid for acute pain syndromes, while transitioning to non-opioid options.
A pain treatment plan should also be initiated early in the course of chronic (long-term) pain management. Longer-term options, combined with alternative treatments such as exercise, physical therapy, TENS therapy, meditation, and or neuropathic drugs for pain may be helpful.
Many of the extended-release formulations of opioid pain medications are only to be used in opioid “tolerant” patients (meaning they have already been using other opioids) and for chronic pain that requires 24-hour, around-the-clock pain management, such as severe cancer pain.
Other medicines such as:
- methadone (Methadose)
- buprenorphine (Sublocade)
- buprenorphine combined with naloxone (Suboxone, Zubsolv)
- naltrexone (Vivitrol)
are used in the treatment of opioid dependence (addiction), either from prescription drugs or illicit narcotics such as heroin6. Sublocade, Suboxone, Vivitrol and Zubsolv are NOT used to treat pain.
Is My Drug a Narcotic?
Below is a list of narcotic drugs (opioid analgesics) available on the U.S. market. The generic names are listed first, with brand name products in parentheses. Follow the link for specific prescription information about dosing, warnings, side effects, and drug interactions. This list may not contain all possible products.
List of Common U.S. Prescription Opioids (Single Agents)
- alfentanil
- buprenorphine injectable (Buprenex)
- buprenorphine transdermal (Butrans)
- butorphanol
- codeine sulfate
- fentanyl (Actiq, Duragesic, Fentora, Lazanda, Subsys)
- hydrocodone (Hysingla ER)
- hydromorphone (Dilaudid)
- levorphanol
- meperidine (Demerol)
- methadone (Methadose)
- morphine (Kadian, MS Contin)
- morphine liposomal
- nalbuphine
- oliceridine (Olinvyk)
- opium tincture, USP (Deodorized)
- oxycodone (Oxaydo, OxyContin, Roxicodone, Xtampza ER)
- oxymorphone
- remifentanil (Ultiva)
- sufentanil (Dsuvia)
- tapentadol (Nucynta, Nucynta ER)
- tramadol (Conzip, Qdolo, Ultram)
List of Common U.S. Prescription Opioids (Combination Agents)
Narcotic analgesic combinations are drugs containing a narcotic analgesic with another class of medicine, such as an analgesic like acetaminophen, ibuprofen or aspirin. They are used to treat moderate to severe pain.
Propoxyphene, found in products such as Darvocet N 100 (propoxyphene and acetaminophen) was taken off the U.S. market in 2010 due to safety and effectiveness concerns.
Follow the links below for specific information about dosing, side effects, and drug interactions for each drug. The generic drug names are listed first, with brand name products in parentheses. This list may not contain all possible products.
- aspirin butalbital caffeine and codeine (Fiorinal with Codeine)
- acetaminophen and benzhydrocodone (Apadaz)
- acetaminophen butalbital caffeine and codeine (Fioricet with Codeine)
- buprenorphine and naloxone* (Suboxone, Zubsolv)
- acetaminophen and oxycodone (Percocet)
- acetaminophen and hydrocodone (Lorcet)
- acetaminophen caffeine and dihydrocodeine (Trezix, Dvorah)
- acetaminophen and tramadol (Ultracet)
- aspirin and oxycodone (Percodan)
- acetaminophen and codeine
- naloxone and pentazocine
*Buprenorphine and naloxone is a combination medicine used for treatment of opioid (narcotic) dependence, not for use as a pain medication.
Uses for Opioids
- Acute Pain
-
Breakthrough pain (for example, cancer pain)
Note: Most dentists and oral surgeons now prefer use of acetaminophen and / or ibuprofen for uncomplicated cases of wisdom teeth removal, which is just as effective as opioid use.13
Common Side Effects of Opioids
Morphine and its derivatives are classified as narcotics analgesics. Narcotics like morphine may cause many different types of side effects, but all cause drowsiness, sedation, and can lead to respiratory depression (difficulty breathing), especially when combined with alcohol or other CNS depressant drugs (which can be fatal).
- Drowsiness and impaired judgment; do not drink alcohol, drive, or operate heavy machinery
- Pruritis (itching)
- Opioid-induced constipation
- Nausea or vomiting
- Withdrawal symptoms upon discontinuation; your doctor may suggest to slowly stop your narcotic to lessen withdrawal side effects
- Tolerance to the pain relief effect can occur over time (meaning you may need a higher dose to get an equal amount of pain control)
- Dizziness, confusion, possibility of falls; may be worse in the elderly
In May 2018, the FDA approved Lucemyra (lofexidine hydrochloride) to reduce the severity of withdrawal symptoms (such as anxiety, nausea, stomach cramps, and sleep problems) and allow a more rapid discontinuation of opioids in adults.
Lucemyra is an oral, selective alpha 2-adrenergic receptor agonist that reduces the release of norepinephrine thought to contribute to opiate withdrawal symptoms. It is NOT a treatment for opioid use disorder (OUD) and is only approved for treatment for up to 14 days.
Learn More: Search for a complete list of your opioid side effects
Fentanyl Abuse
Fentanyl is major factor in opioid overdose deaths. Prescription fentanyl is a useful and potent synthetic opioid pain medication with legitimate medical uses. However, illicit forms of fentanyl and an analog, carfentanil, are being abused on their own or laced into streets drugs such as heroin and illegal Oxycontin. Much of this dangerous fentanyl is brought in from China and Mexico. Overdoses have occurred, often when the user was not aware that fentanyl was laced in the street drug they purchased.
In 2020, more than 56,000 people died from overdoses in the U.S. involving synthetic opioids, including illicitly manufactured fentanyl. More recent data is shocking - in 2022 over 110,000 people were reported to have died from an overdose, of which almost 69,000 were due to synthetic opioids.
Related: Fentanyl Abuse: Top 11 Facts About This Potent and Deadly Opioid
Guidelines on Safe Opioid Use
Tackling the opioid epidemic requires a multi-pronged approach. Industry, patients, prescribers, and insurance payers all need to work together to address this pressing problem.
The American Medical Association (AMA) has developed "End the Epidemic" an online, evidence-based resource that can help to treat patients effectively with pain and substance use disorders.8
The Centers for Disease Control and Prevention (CDC) has developed educational programs for prescribers on the proper use of opioids, prescribing and discontinuation entitled 2022 CDC Guideline for Prescribing Opioids for Chronic Pain.9
The Veterans Administration has also implemented a Clinical Practice Guideline for Opioid Therapy for Chronic Pain.10
In September 2018, the FDA announced the release of the final Opioid Analgesic Risk Evaluation and Mitigation Strategy (REMS).11 The REMS plan communicates the serious risks of opioid pain medications to patients and health care professionals.
Rescheduling of Opioids to Ease Misuse and Diversion
Tramadol
Tramadol (Conzip, Qdolo, Ultram), a common pain medication, has been linked with drug abuse and misuse, dependence, and even fatal overdoses. To address these concerns, in 2014 the DEA placed all forms of tramadol into schedule IV of the Controlled Substances Act (CSA).
Previously, tramadol was thought to be a lower risk drug for abuse and overdose and was a controlled substance in only a few U.S. states. Tramadol prescriptions may now only be refilled up to 5 times in a 6 month period after the date the prescription was first written. After 5 refills or 6 months, whichever occurs first, a new prescription is required from the physician.
Even though tramadol may have other pain mechanisms in addition to a narcotic effect, people with a history of drug abuse may be at a greater risk of addiction. Tramadol is related to other opioids like codeine and morphine and can lead to psychological and physical dependence, drug-seeking behavior, addiction, and withdrawal symptoms. Withdrawal symptoms may occur if tramadol is abruptly stopped. Dose reduction of long-term tramadol use should be directed by a doctor.
Hydrocodone
Hydrocodone and oxycodone have been among the most common prescription painkillers abused in the U.S., and they are frequently prescribed in higher amounts than needed for minor pain. Hydrocodone is also used in cough suppressants. These drugs may also contain a non-opioid analgesic, like acetaminophen or ibuprofen, or a cough and cold product.
- In October 2014, hydrocodone was rescheduled from schedule III to schedule II of the Controlled Substances Act.
- Patients now need a new prescription from their doctor each time they renew their medication for any hydrocodone product; refills are no longer allowed to be ordered for hydrocodone.
- The DEA put this rule into place to help curb abuse, diversion, and encourage patients and healthcare providers to consider other, more safe ways to combat pain.
Can I Become Addicted to an Opioid?
If and how quickly you become addicted depends on many factors. Addiction is a multi-faceted condition that involves:
- personality and behaviors
- brain chemistry
- age
- environmental and family surroundings
- types of drug abuse
- past personal and family history of drug abuse
While one individual may use a drug once or many times and not become addicted, another person may overdose with the first use, or become addicted quickly. Each person varies in their susceptibility to drug addiction.
Any opioid-based painkiller can lead to addiction. Narcotics often involved in prescription painkiller addiction and overdose include:
- morphine
- oxymorphone
- oxycodone (Oxycontin)
- hydrocodone
- codeine
- methadone
- fentanyl
Also concerning is that many of these medications may also contain acetaminophen (Tylenol) which in itself can be toxic to the liver at excessive doses. Codeine is also found in headache combinations such as Fioricet with Codeine.
- Always store prescription narcotics safely in your home away from children, pets and teenagers. If needed, lock them up securely and out of reach.
- Most adults should not exceed 3,000 to 4,000 milligrams (3 to 4 grams) of acetaminophen over a 24-hour period. This includes all medicine: any other combination medicines that may contain acetaminophen, prescription or over-the-counter medications.
- All combination pain prescription products now only contain 325 mg acetaminophen per tablet (down from 500 mg per tablet).
- DO NOT exceed the recommended 24 hour dose of acetaminophen (maximum of 4 grams) from all products (prescription and over-the-counter).
- Drinking alcohol while you are taking acetaminophen may be toxic to your liver. Severe liver damage may occur if you take 3 or more alcoholic drinks every day while using a product containing acetaminophen. Talk to your doctor about this interaction.
What Is Naloxone (Narcan)?
A narcotic reversal agent called naloxone (Narcan, Narcan Nasal, Kloxxado, Zimhi) can be a life-saving drug for patients who overdose on narcotics.
All narcotic painkillers will produce various levels of central nervous system (CNS) depression like drowsiness and sedation. One of the most serious concerns with excessive opioid use is slowed breathing (respiratory depression). When narcotics are combined with other CNS depressants, like alcohol or benzodiazepines, severe, possibly fatal respiratory depression can occur.
If you believe someone has overdosed on narcotics, call 911 immediately. Naloxone can be kept by family members or caregivers for administration in emergencies. It is available at most US pharmacies without a prescription. Be sure you learn how to use it before an emergency and discuss this with your healthcare provider, if needed.
Based on recommendations from a Medical Advisory Committee to the FDA, naloxone is expected to be available over-the-counter without a prescription in 2023.
Drug Testing for Narcotics
Prescription and illicit opioids are a regular component of workplace drug testing in the U.S. Urine drug screening may also take place in the clinic during management of pain therapy.
Physicians who manage pain may engage some patients in a treatment plan that includes urine drug screening to monitor their opiate management. These laboratory results can provide the doctor with objective data on which to make therapeutic and diagnostic decisions, identify misuse or diversion, and assess compliance. Doctors should describe the screening and frequency at the initial evaluation. Patients must be willing to participate in the screening to help manage their pain.
Which drug test is used for workplace drug screening is dependent upon the private employer, federal requirements, or other workplace guidelines that may be in place. Patients should inform the lab of the prescription, over-the-counter, and herbal medications they currently take.
- Employers may use a standard five-panel test of commonly abused drugs such as marijuana (THC), cocaine, PCP, opiates (e.g., codeine, morphine, methadone) and amphetamines like methamphetamine.
- Employers may also elect to use a multi-drug panel test that also includes other prescription drugs, such as hydrocodone, oxycodone, hydromorphone, benzodiazepines, or barbiturates.
- They may also select to screen for alcohol in the sample. Other more recent drugs of abuse or designer drugs, such as MDMA (Ecstasy) may be included.
Drug Detection Time in Urine
Note: All times are approximate and may vary based on patient-specific drug metabolism, drug half-life, patient’s medical conditions, other drug treatments, and frequency of drug ingestion.12
| Drug | Approximate Retention Time (general guidelines) |
|---|---|
| Amphetamines | 48 hours |
| Barbiturates | Short acting, such as secobarbital: 24 hours Long acting, such as phenobarbital: up to 3 weeks |
| Benzodiazepines | Roughly 3 days if short-term dose Up to 6 weeks after extended use (or abuse) |
| Cocaine metabolite | 2 to 4 days |
| Ethanol (alcohol) | 2 to 4 hours |
| Methadone | About 3 days |
| Opiates | Up to 3 days (morphine/codeine) |
| Cannabinoids | Moderate smoker (3-4 times/week): 5 to 6 days Heavy smoker (smoking daily): 10 days or longer Retention time for chronic smokers may be 20 to 28 days |
| Phencyclidine | Roughly 8 days Chronic use: up to 30 days |
Source: Heit HA, Gourlay DL. Urine drug testing in pain medicine. J Pain Symptom Manage. 2004 Mar;27(3):260-7.
Read More
Learn more
- Bath Salts Drug
- Can a Drug Test Lead to a False Positive?
- Cannabis: Uses, Effects and Safety
- Cocaine
- Devil's Breath: Urban Legend or the World's Most Scary Drug?
- Do blood pressure drugs interact with alcohol?
- Dosage Charts for Infants and Children
- Drug and Substance Abuse
- Ecstasy
- GHB or Gamma-Hydroxybutyrate
- Hashish
Treatment options
- Medications for Angina
- Medications for Back Pain
- Medications for Breakthrough Pain
- Medications for Chronic Pain
- Medications for Drug Dependence
- Medications for Muscle Pain
- Medications for Neck Pain
Care guides
- Acute Coronary Syndrome
- Angina
- Ankle Sprain
- Back Pain
- Barbiturate Use Disorder
- Benzodiazepine Use Disorder
- Caffeine Use and Athletic Performance
Symptoms and treatments
Medicine.com guides (external)
Sources
- Dowell D, Ragan KR, Jones CM, et al. CDC Clinical Practice Guideline for Prescribing Opioids for Pain — United States, 2022. MMWR Recomm Rep 2022;71(No. RR-3):1–95. DOI: http://dx.doi.org/10.15585/mmwr.rr7103a1
- Dowell D, Ragan KR, Jones CM, et al. Prescribing Opioids for Pain — The New CDC Clinical Practice Guideline. N Engl J Med 2022; 387:2011-2013
DOI: 10.1056/NEJMp2211040 - The Atlantic. A Brief History of Opioids: Pain, Opioids, and Medicinal Use.
- Fudin J. Abuse-deterrent Opioid Formulations. Purpose, Practicality, and Paradigms. Pharmacy Times. January 27, 2016. https://www.pharmacytimes.com/contributor/jeffrey-fudin/2015/01/abuse-deterrent-opioid-formulations-purpose-practicality-and-paradigms
- Moorman-Li R, Motycka CA, Inge LD, et al. A Review of Abuse-Deterrent Opioids For Chronic Nonmalignant Pain. Pharmacy and Therapeutics. 2012;37(7):412-418.
- Al-Hasani R, Bruchas MR. Molecular Mechanisms of Opioid Receptor-Dependent Signaling and Behavior. Anesthesiology. 2011;115(6):1363-1381. doi:10.1097/ALN.0b013e318238bba6
- Compton WM, Jones CM, Baldwin GT. Relationship between Nonmedical Prescription-Opioid Use and Heroin Use. N Engl J Med 2016; 374:154-163.
- American Medical Association (AMA). End the Epidemic. Task Force Recommendations. https://www.end-opioid-epidemic.org/
- U.S. Centers for Disease Control and Prevention (CDC). CDC Guideline for Prescribing Opioids for Chronic Pain. https://www.cdc.gov/mmwr/volumes/71/rr/rr7103a1.htm
- Department of Veterans Affairs. Dept. of Defense. Clinical Practice Guideline for Opioid Therapy for Chronic Pain. https://www.healthquality.va.gov/guidelines/Pain/cot/VADoDOTCPG022717.pdf
- FDA’s Opioid Analgesic REMS Education Blueprint for Health Care Providers Involved in the Treatment and Monitoring of Patients with Pain. US Food and Drug Administration (FDA). https://www.fda.gov/media/99496/download
- Heit HA, Gourlay DL. Urine drug testing in pain medicine. J Pain Symptom Manage. 2004 Mar;27(3):260-7. doi: 10.1016/j.jpainsymman.2003.07.008
- Moore PA, Hersh EV. Combining ibuprofen and acetaminophen for acute pain management after third-molar extractions: translating clinical research to dental practice. J Am Dent Assoc. 2013 Aug;144(8):898-908. doi: 10.14219/jada.archive.2013.0207
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
