Insertion of a Heart Failure Monitoring System
Medically reviewed by Drugs.com. Last updated on Jun 5, 2024.
AMBULATORY CARE:
What you need to know about the insertion of a heart failure monitoring system:
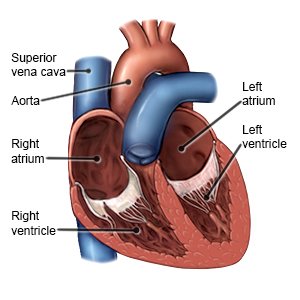
A heart failure monitoring system measures pressure near your heart. It does this through a sensor that is inserted (placed) in your pulmonary artery. Your pulmonary artery brings blood from your heart to your lungs. The sensor is placed during a heart catheterization. Pressure readings are sent to your healthcare provider through the internet. This information can help your healthcare provider identify and treat heart failure problems early. Early identification and treatment can prevent your heart failure from getting worse. It can also prevent or decrease hospital stays.
 |
How to prepare for the procedure:
- Your healthcare provider will tell you how to prepare. He or she may tell you not to eat or drink anything after midnight on the day of the procedure. Arrange to have someone drive you home when you are discharged.
- Tell your provider about all medicines you currently take. He or she will tell you if you need to stop any medicine for the procedure, and when to stop. He or she will tell you which medicines to take or not take on the day of the procedure.
- Contrast liquid will be used to show the parts of your heart more clearly in pictures. Tell your provider if you have had an allergic reaction to contrast liquid.
- You may need blood or urine tests before your procedure. Talk to your healthcare provider about these or other tests you may need.
What will happen during the procedure:
- You will be given medicine to help you relax. You will receive local anesthesia that will numb the area where the catheter will be placed. You will be awake during the procedure so that your healthcare providers can give you instructions. You will need to let them know if you have any discomfort.
- Your healthcare provider will insert a catheter into a vein in your leg or neck. He or she will use an x-ray to guide the catheter to your heart. Contrast liquid will help heart vessels, muscle, or valves be seen more clearly. You may get a warm feeling or slight nausea right after the liquid is injected. This is normal, and will pass quickly. Your provider will place the sensor device in the artery. The catheter will then be removed.
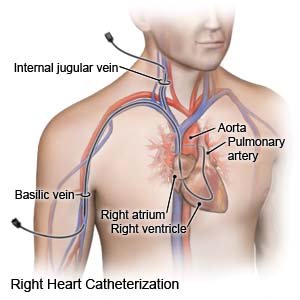
- Pressure will be applied to the incision site for at least 30 minutes to help decrease the risk for bleeding. A collagen plug or other closure device may be used to close the site. The site will be covered with a pressure bandage or other pressure device to help stop any bleeding.
What to expect after the procedure:
- You will be attached to a heart monitor until you are fully awake. Healthcare providers will check your pressure bandage often for bleeding or swelling.
- You will need to lie flat with your leg or arm straight for 2 to 4 hours. Do not get out of bed until your healthcare provider says it is okay. Arm or leg movements can cause serious bleeding. When your providers see you are okay, you may be able to go home.
- You may have pain, swelling, or bruising at the catheter site for a few days.
Risks of the procedure:
During the procedure, the catheter may tear a vein and cause bleeding. An air bubble may enter your lung, or your lung may collapse. You may have a heart attack. After the procedure, you may have bleeding or develop an infection. You may have damage to a heart valve, or a fistula (abnormal opening) may form between an artery and vein. You may have irregular heartbeats that cause dizziness or fainting. You may get a blood clot in your leg or arm. These problems may become life-threatening.
Call your local emergency number (911 in the US) if:
- Your catheter site does not stop bleeding even after you apply firm pressure for 10 minutes.
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
- You feel lightheaded, short of breath, or have chest pain.
- You cough up blood.
Seek care immediately if:
- The catheter site is swollen and filled with blood or is bleeding.
- The area where the catheter was placed is swollen and filled with blood or is bleeding.
- The leg or arm used for the procedure becomes numb or turns white or blue.
- You have a severe headache or feel dizzy.
- You have vision changes or loss of vision.
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
Call your doctor if:
- You have a fever.
- The skin around your catheter site is red, swollen, or has pus coming from it.
- Your skin is itchy, swollen, or has a rash.
- You have questions or concerns about your condition or care.
Limit activity as directed:
- You may feel like resting more after your procedure. Slowly start to do more each day. Rest when you feel it is needed. Ask your healthcare provider how long you need to limit movement and avoid certain activities. He or she will tell you when you can return to your usual daily activities.
- If the catheter was placed in your wrist, do not place pressure on your arm, hand, or wrist. Do not push, pull, or lift anything heavy with that arm.
- If the catheter was in your groin, limit stair climbing as directed for 48 hours. Support the catheter site with your hand if you need to cough.
Drink liquids as directed:
Liquids help flush the contrast liquid out. Ask your healthcare provider how much liquid to drink each day, and which liquids to drink.
Care for the procedure area:
Your healthcare provider will give you specific instructions. This will include when you can take a shower. Do not soak in a bathtub, pool, or hut tub until your provider says it is okay. Check the area each day for signs of infection, such as swelling, redness, or pus.
Carry your medical identification card with you at all times:
You will be given a temporary card before you leave the hospital. Your permanent card will be mailed to you. The information on the card can help healthcare providers keep you safe in an emergency. It can also help them keep you safe during an x-ray, CT, or MRI.
Bring your equipment with you when you travel:
Remove the antenna and cords from the PES before you pack it. You can pack the equipment in its case, or you can use your own case. Carry on the equipment with you when you travel by airplane.
Follow up with your doctor or cardiologist as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2024 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
